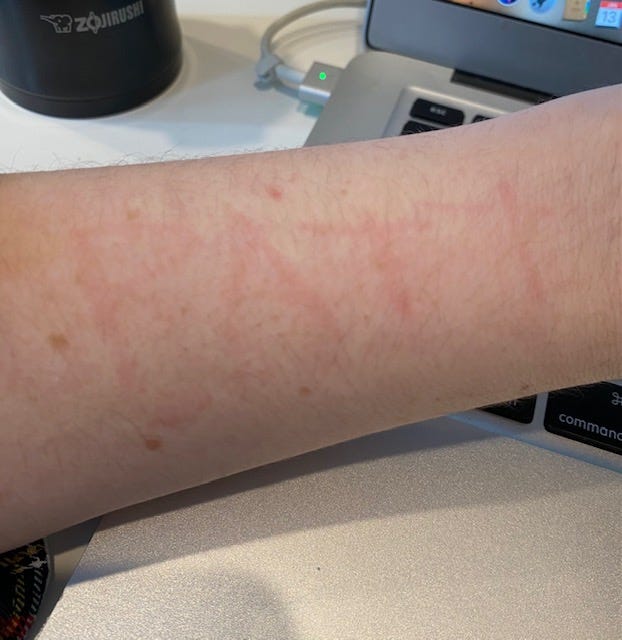
Six months into the pandemic, I started getting hives. They weren’t the circular, one-off kind I was used to getting. These were thick, red slashes that spread across my body multiple times a day (and in the wee hours of the night). I googled “hive stripes” and learned that I probably had a condition called dermatographia. Street name: skin writing.
People with dermatographia react to the faintest scratch. Trace your name on your arm using your nail, and if you have dermatographia, the letters will appear as welts. Other everyday interactions, like fabric rubbing against your back or a countertop pressing against your stomach, can also trigger a response. Me? I was irritated by everything. The dog leash wrapped around my wrist. The bag slung over my shoulder. My bra.
I read that dry skin can make dermatographia worse, so I started moisturizing like a madwoman. I switched from Dove soap to unscented Dr. Bronner’s. I went from taking two hot showers a day to one. I covered my body in almond oil at the recommendation of a blogger who turns her dermatographia into body art. Nothing worked.
After months of sleepless, itchy nights, I went to see a dermatologist. She scratched a line down my back using a wooden stylus, observed the subsequent welt, and confirmed my diagnosis. “It could be a stress response,” she told me. I’d read as much online. The cause of dermatographia is a mystery, but some experts believe it can be brought on by emotional disturbances. “It’ll probably go away on its own.”
Fast forward to March 2021, when vaccines were rolling out and hope was in the air for the first time in a long time—and the hives disappeared.
Caregivers are a stressed bunch. According to the AARP, one in four find it difficult to tend to their own health, and a similar percentage report that caregiving has made their health worse. A 2007 study by Ohio State University, in conjunction with the National Institute on Aging, concluded that adult children caring for their parents may see their life span shortened by four-to-eight years. For people of color, the health consequences of caregiving are even worse, compounded by the effects of systemic racism.
I know that I’m lucky, all things considered. I have health insurance and access to good doctors, and barring unpredictable upsets, I’m able to keep my caregiving duties (which, at this stage, often amount to “hanging out with my dad”) to about 18 hours a week. Yet, even with all my privilege, being a caregiver has negatively impacted my health. I’m more exhausted than other child-free 39-year-olds I know. I’ve had an unexplained cough for years. (I’ve seen three pulmonologists, two gastroenterologists, an ENT, an allergist, and an acupuncturist, and the only diagnosis I’ve received is “habit cough.”) And, well, you’ve heard about my dermatographia, right?
I recently had a helpful talk with Martin Picard, PhD, an associate professor at Columbia University's Irving Medical Center, about how chronic stress impacts our well-being on a cellular level. He’s a convincing proponent of what he calls an “energetic perspective” of health—the view that our longevity is, above all, tied to our mitochondria (the organelles that create energy in our cells). Mess with your mitochondria, the theory goes, and you mess with your life.
“Think of your cells as a government,” Dr. Picard explained. “You receive the signal that there’s a big threat somewhere on the planet and you’re like, ‘Oh, we might go to war.’” Keeping with this analogy, you take all of your financial resources and manpower—your energy—and you put them into the army at the expense of everything else (health care, education, etc.).
“Now you’re going to be ready for war, that’s great,” Dr. Picard said. “But you’re going to suffer consequences a decade or two later.” That’s the same tradeoff mitochondria make when they’re forced to respond to chronic stress: They divert energy to prepare for what they’ve deemed a threat—and, as a result, they neglect the parts of their job that might promote health and longevity.
The good news is, there are ways to optimize your mitochondria. You can move more, for example. Or, you can do things that bring meaning to your life, that inspire you.
“It’s not about pleasure and excitement,” Dr. Picard said. “It’s about finding connection and purpose.”
The caregiving space puts a lot of emphasis on the importance of self-care, and that’s a good thing—we need sleep, exercise, and breaks from our 24/7 worrying. But, colloquially, “self-care” has come to mean so much that, to me, it now means very little. Self-care is a bubble bath. It’s a hike. It’s a night out. It’s an evening in. I’m reminded of when my boyfriend used to call aimless Saturdays “do what you feel days.” After four years of emotional turmoil, I don’t really want to “do what I feel”—I just want to do what needs to be done. I want to get my health back on track. I want to make up for lost time.
As it turns out, even my mitochondria expect more introspection from me. Who am I? What inspires me? I’m not sure anymore, but I know that the hole I’m climbing out of is dark and slippery, and if I ever want to find myself on steady ground, I may need to feel my way out.