The Diagnosis Doctors Don't Want to Give
It can take years to get a dementia diagnosis, in part because physicians aren’t prepared to give it. What’s the solution?
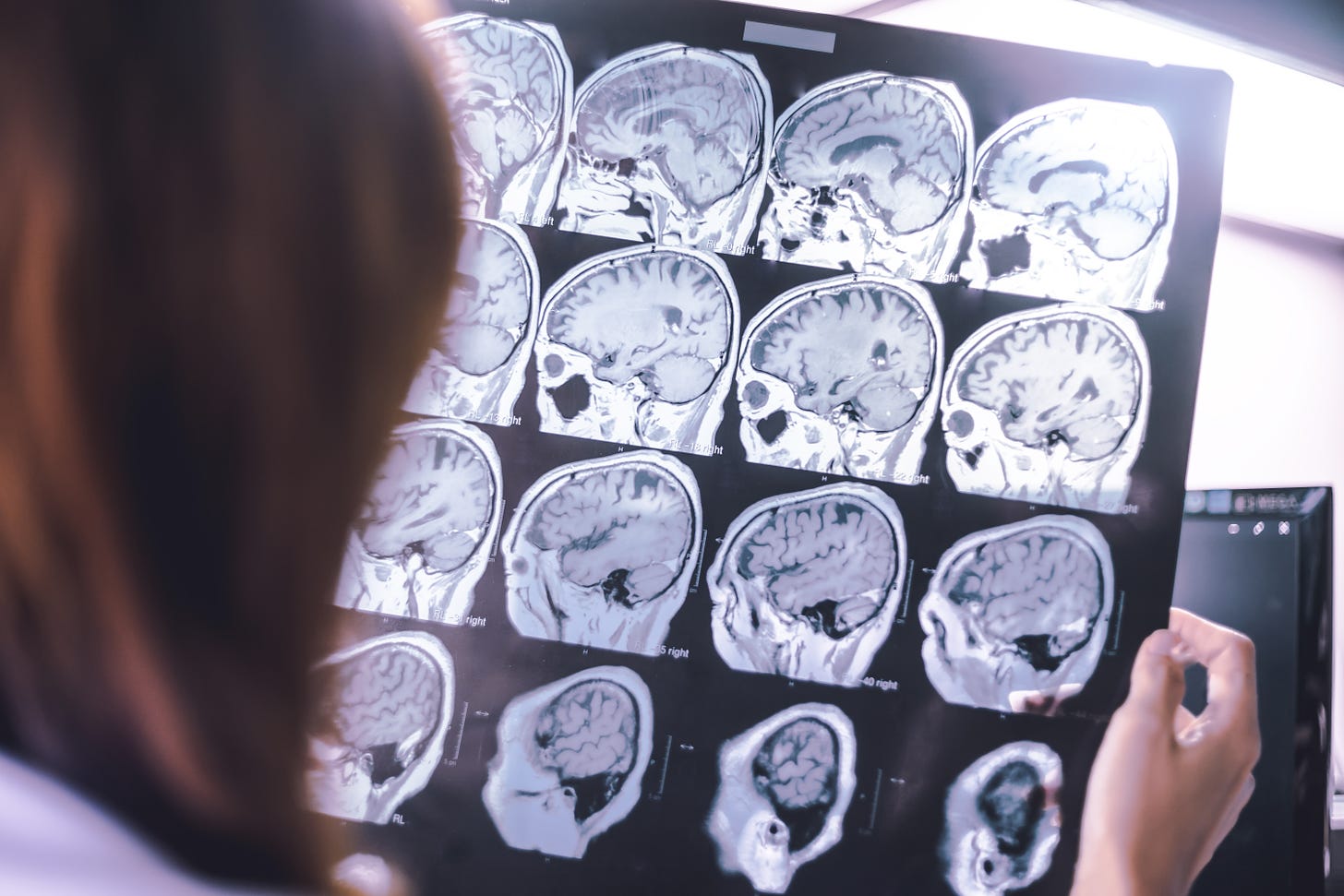
My father was diagnosed with mild cognitive impairment (MCI) in October 2018. I remember feeling relieved—euphoric, even—when the neurologist delivered the news. “Daddy, this is great!” I said. “I thought he was going to tell us you had dementia.” Dementia seemed like a death sentence; mild cognitive impairment, on the other hand, sounded manageable. It was mild.
We went to an Italian restaurant for lunch, then returned to my dad’s house, leftovers in hand, to rest. An hour later, maybe less, my father pulled a doggy bag from his fridge. “What’s this?” he asked. He didn’t remember eating.
The long road to a diagnosis
It can take years for a patient to get diagnosed with dementia, and that’s if they get diagnosed at all. “We know that only about half the folks living with Alzheimer’s [in the U.S.] right now actually have a diagnosis,” says Beth Kallmyer, MSW, vice president of Care and Support for the Alzheimer's Association. The global estimate is even worse. According to the 2021 World Alzheimer’s Report, 75 percent of all cases go undiagnosed (or up to 90 percent in low- and middle-income countries).
There are a number of explanations for why dementia lives in the diagnostic shadows. The most obvious is that it’s scary—people don’t want to know they have it. “It’s a feared disease,” says Kallmyer. “People are very concerned, as they age, about needing the level of help that you need when you’re living with dementia.” They may notice they’re more forgetful or confused than usual—that they can no longer follow a simple recipe or are getting lost on the way to the grocery store—but they’re too terrified to seek a professional opinion as to why that is. (It’s also possible they lack insight into their condition, a symptom of dementia known as anosognosia.)
That’s the patient-centric side of the diagnosis problem. The physician-centric side is arguably thornier. For starters, dementia is still a clinical diagnosis. Doctors arrive at it through a series of mental status tests, physical and neurological exams, and brain imaging. “It’s a rule-out,” Kallmyer says. “There isn’t a blood test the doc can give and say, ‘Yep, the test indicates that this is what’s going on.’” Because of that, some physicians avoid diagnosing their patients until they’re further along in the disease, especially if those patients are younger than usual (my dad was in his early sixties). “If they can’t be 100 percent sure, then I think they’re reluctant to give this kind of bad news,” Kallmyer says.
It doesn’t help that most doctors who treat dementia patients are primary care physicians rather than, say, neurologists or geriatricians. One study found that 85 percent of people diagnosed with the disease were assessed by a non-specialist. The problem is, PCPs often lack the experience and time necessary to make an appropriate diagnosis. “Dementia is complicated,” Kallmyer says. “And frankly, the primary care doctor’s 15-minute appointment model doesn’t [work].”
Perhaps the most surprising reason a diagnosis might get delayed, at least for those of us who are new to dementia care, is a sort of nihilism in the medical field. What’s the point, some doctors figure. There’s no cure for dementia.
Why a diagnosis matters
Myra Garcia was a vice president at a university in California when she started struggling to keep up at work. Her boss couldn’t quite understand the problem. “Maybe she thought I wasn’t paying attention, or that I was just doing things the way I wanted to do them,” Myra recalls. Whatever the case, “she was not happy with me.” Myra, then in her late fifties, was invited to stay on at the university, but in a different, less prominent, role. She took the offer.
“At the time that was all happening, I was just looking for answers,” Myra, now 64, says. She consulted her GP twice and, after being told repeatedly that she was “fine,” sought the opinion of a neurologist, who diagnosed her with attention deficit disorder. She started medication and monthly therapy, and for a while things seemed to be going okay. But then she landed another VP position, and her professional situation unraveled again. “I only lasted three months,” she says. “I couldn’t do the work. That was really painful.”
She fell into a depression and didn’t reach a turning point until she sought help from a neuropsychiatrist. This time, Myra says, her diagnosis was “abundantly clear”: She had early-onset Alzheimer’s. That was two years ago.
There is no cure for dementia, it’s true, but there are benefits to getting a diagnosis. “If you have a progressive, fatal disease, you should know that, and the people around you should know that,” Kallmyer says. “Because that gives you and your family members and caregivers an opportunity to get educated about it and put a plan together. How’s care going to go? What sort of advance directives do you want to put in place?”
A diagnosis can also ease family tension (it might help a wife understand why her husband has been acting so strange, for example) and minimize personal frustration. “I felt vindicated after my diagnosis, like, I’m not just making this up, this is real,” Myra says. “I also felt empowered.”
She started clinical trials at the University of Southern California, joined the Alzheimer’s Association (she’s now on the board of the Southland Chapter), and left the traditional workforce to focus on more manageable activities, like singing in multiple choirs, volunteering at a memory-care unit, and playing golf with her husband. (“We’ve agreed that I don’t necessarily have to count,” she says.) Her current level of cognitive functioning won’t last forever, and Myra knows that. But for now, she says, “I’m going to do everything that I can to live a full and wonderful life.”
The future of diagnosing dementia
Many researchers believe that, in as little as a year, we’ll have a blood test that detects Alzheimer’s biomarkers, which means that at least one barrier to diagnosing the most common form of the disease will be lifted (and that earlier, even presymptomatic, detection may be possible).
There are also potential new Alzheimer’s treatments in the works, like the drug lecanemab, which targets amyloid plaques (one possible cause of the disease) in the brain. According to early data from pharmaceutical companies Eisai and Biogen, lecanemab can slow the rate of cognitive decline in people with early-stage Alzheimer’s by 27 percent over the course of 18 months. (Last year’s buzzy aducanumab also worked to weed out the dreaded protein clumps, but it didn’t show any clinical benefits in trials, which is why its FDA-approval was so controversial.)
Lecanemab isn’t a cure—or even a surefire treatment (it still awaits peer review). And it’s certainly not without its skeptics: The drug would need to be administered via monthly infusions, which are timely and costly; it may cause brain swelling and bleeding—side-effects that arguably outweigh the benefits; and it's only been shown to help people who are at the very start of the disease, which requires early detection.
But experts are banking on the idea that new treatments, coupled with diagnostic advancements, can help create a shift in the perception of dementia, transforming it from dead-end disease to a crisis worth confronting. “We have to make the field exciting,” says Serge Gauthier, M.D., lead author of the 2021 and 2022 World Alzheimer’s Reports. “‘There are new treatments! There are new diagnostic tests!’”
Dr. Gauthier’s hope is that Alzheimer’s eventually “moves a bit like diabetes,” he says. “Where you catch it early enough—when you’re presymptomatic, very mildly symptomatic—and delay progression to a more advanced stage.”
Finding hope
After my dad’s MCI diagnosis, I started seeing a social worker for support. “He doesn’t have MCI—he has dementia,” she said. “A lot of doctors just won’t say the word.”
What I didn’t understand on the day of my dad’s diagnosis—and what the doctor didn’t explain to me—is that there’s a fine line between MCI and dementia. “The key difference is meant to be that, in MCI, the person has cognitive impairment but largely functions independently in daily life, whereas with dementia, there’s [also] evidence of loss of independence and difficulties in daily functioning,” says Mayo Clinic neurologist David S. Knopman, M.D. “But that line in the particular individual can be a little uncertain.” And yes, he says, people are sometimes diagnosed with MCI when they, in fact, have dementia. (MCI doesn’t always lead to dementia.)
Based on my father’s condition and what I gathered from his wife before she left him, an MCI diagnosis might have been appropriate two or three years prior to that date in October, when he first showed signs of memory loss and confusion. But on the day of his diagnosis, he was no longer able to manage bills or medication, he couldn’t keep track of meals, and he didn’t know the month or year. Any hope that he didn’t have a progressive disease was false.
There’s not much I would have done differently had my father gotten a dementia diagnosis right out of the gate. After learning more about MCI and reading between the lines, I mobilized accordingly—hired his divorce attorney, arranged for him to move closer to family, worked with his wife to sell their house. But the inadequacies of our current dementia-care system are bigger than any one person’s story. Our global population is aging, and more people than ever are poised to develop dementia. How can we make certain they get the care they deserve if they can’t even get a timely diagnosis?
“I’m more optimistic now than ever about getting doctors interested,” Dr. Gauthier tells me. He sees the potential for Alzheimer’s to undergo the same revolution in treatment that transformed the outlook on multiple sclerosis. “Think of Alzheimer’s as something that will become a chronic illness that can be detected earlier and managed better for a longer period.”
It can be hard for some caregivers, myself included, to accept a rebrand of Alzheimer’s that paints it as anything other than a merciless disease, or to celebrate medical advancements that fall short of a cure. But perhaps there’s value to progress that begets more progress. If a groundswell of enthusiasm motivates a generation of doctors to engage more critically with dementia, that would be something of a win. If not for my father, then for the ones who come next.


My older partner had dementia. When he first started having weird memory lapses, he went to his PCP who told him, "Everyone your age forgets things." He was 75, super active, still working etc. The problem was that a few months later, he had 2 minor surgeries within a month and he went from being maybe 80% of himself to being 50% of himself within a few weeks--because it turns out that anesthesia can really screw up your brain if you're having cognitive issues. I can't say now that he wouldn't have had the surgeries had we known that, but we would have talked a lot more with his doctors ahead of time and made a much more informed decision. By the time he got the diagnosis a few months later, the dementia was already classified as moderate. Thankfully, that PCP is now retired, but I still wonder if the progression would have been any different had his doctor taken him seriously at the beginning. As it was, the surgeries definitely accelerated his decline, and he died 2 1/2 years after he was formally diagnosed. I'm sorry you have to go through this with your dad.
This is fascinating -- I had no idea this was such an under-diagnosed disease. It’s upsetting when you think about what doctors are trained to fixate on (like telling pregnant women they gained too much weight). Gotta love the American healthcare system 🇺🇸